HOME CARE SUPPORT INFORMATION:
|
 |
| Fig 1. Wheelchair ramp |
In our case, a friend who was physical therapist living nearby helped me obtain two 10 foot 2"x4"s (rails) and a surface sheet of 3/4" plywood, 4 foot x 8 foot. We cut the sheet to make a three-foot wide ramp. Then we cut a 2-foot x 3-foot plywood section from the unused plywood to complete the surface of the 10-foot long ramp supported by the two rails. You need to cut the ends of the rails to be parallel to the ground. At the top, the rails will rest on the next to the top step. Most lumber companies can make the lumber cuts for assembly, but they must have the total number of the stairs including the one to enter the house so they can trim the ends of the rails to match the ground. I found that it was easy to assemble the pieces with grabber (drywall) screws. Then you fasten 1" x 2" (finished) rails on each side to keep the wheelchair on the ramp.
Night Light
You must plan for light at night to care for the patient. You can place a low watt or a compact fluorescent bulb in the bathroom and leave it on for a night light. There are night-lights, which plug into the wall outlet that turn on automatically at night, but these can be somewhat expensive and the bulbs don’t last very long.
Movement in the House
It is best to measure the width of the wheelchair you are going to use to see that it will fit through the doors in the house. You may find that the larger wheelchairs will not fit into the bathroom, so you should plan on a smaller wheelchair with removable arms. In some cases, you may wish to remove a door if it is a very tight fit. Expect some paint scratches, but they can be easily repaired. There are different widths of wheelchairs, which will be discussed below.
Wheelchairs
 |
| Fig 2. Primary wheelchair |
- My primary wheelchair is wide and more comfortable for my wife to sit in over long periods. It is a Sun Mark #0417 (Figure 2). The seat is 18" wide and 26" high above the floor. It was used. Others like the Fuller appear adequate with the same seat width. New larger units have a cost range from $300 to $700.
Some wheelchairs have meal tray accessory that you can buy that snaps onto the wheelchair handles for someone who cannot sit at a table. Since my wheelchair was second-hand, no tray was available. I made a simple food tray out of ¼" Masonite. I used Velcro strips stapled to the Masonite to secure it to the wheelchair handles on each side. To keep the tray from slipping forward, I drilled a small hole in the back on each side and then used a small string threaded through the holes and tied around the back of the chair. I covered the Masonite with self-stick plastic drawer liner to protect the surface from waste spills. It has worked just fine.
- I have a secondary chair for transferring my wife in close quarters, like the bathroom where the wider one cannot navigate. It has proven very valuable. The chair is the right height so we can use a transfer board to move my wife over the edge of the bathtub for bathing. This wheelchair is a "must" in the case of transfer in and out of the car. Both of these transfers will be describe below. To me, no other chair seems to fit the door space lying outside the front seat of the car. It is portable, but the handle extensions do not fold. The arms fold away permitting me to swing my wife straight into the front seat by using a sliding board. In tight places it is very important to have the chair with folding arms. It has a soft padded seat with a width of 16" and can be folded put into the trunk. It was used. Manufacturer: Breezy by Quickie, Quickie Sunrise Medical, Quickie Designs Inc., 800 456 8165.
- The third wheelchair is portable so that it can be placed in the car trunk, but the arms do not fold which makes it a little difficult for my wife to be seated from a standing position. The seat is 23" wide. It was used. A similar unit is sold as the Deluxe Travel Chair by Dr. Leonard's Medical Catalog, 800-785-0880. Cost about $200.
Furniture Adjustments
In some cases a wheelchair will not be level with the another chair that you want to transfer your loved one to. In our case, we have a reclining chair that my wife uses most often for sitting in the living room. It is difficult to use a sliding board or otherwise move someone if the two chairs are not at the same level. I solved this problem by raising the level of the recliner by placing 2"x4" pieces, lying flat under the frame to give the proper height. The pieces are spaced by short blocks and tied together with a few drywall screws to provide a solid short platform for the chair. The 2"x4" pieces were extended beyond the back of the chair, and screws were used to attach the platform to the chair so that the chair would not tip over in the reclining position when it was raised on the platform.
PERSONAL ARTICLES AND CLOTHING
Before you move your loved one into the house, you should have special articles in place. Items in the following list will last about a month and have been tailored to my experience. Obviously, each case requires some tailoring to match the specific needs. For example, if your loved one can use the toilet, they will not need briefs. This list is tailored to my wife's needs as a bedridden person from a stroke.
Shoes
Low cost (K-MART type about $25) athletic walking shoes should fill the bill, but the shoe should cover and support the ankle.
Nightgown
Your loved one needs about three gowns that button down the back for sleeping in. I used a low priced cotton housecoat (K-MART type about $15 each) with buttons in the front that I reversed so the buttons were in the back. This gown must come open from the back in order to slip the brief under the patient when they are lying in bed. Hospital gowns are also suitable.
Briefs
These act as a diaper for those who can not use a regular toilet. There are many types, and you may get the one that suits you in cost and function by asking people in the rest home or hospital. If the brief has a large containment area, it will nearly always last all night, thus, giving you and your loved one a good rest. In my case, I use a brand called Tena which comes in 40 pieces to a box. I use about two boxes a month at a total cost of about $52 per month. A local drug company (Superior Pharmacy 801-266-9999) delivers the package to our door. I will discuss the application later.
Ointment
This is used to protect against bed sores which are nasty things to cure. Apply this ointment to the buttock when you change the brief. Urine can irritate the skin making it red and it is easy for sores to start. I have used two kinds of ointment, and both work well: A+D Original Ointment (Schering-Plough Health Care Products, about $4.00), and Vitamin A & Vitamin D Ointment (Fougera under $2.00). I use about three tubes a month and have applied it, along with baby powder, on the brief change for over two years and have not seen bed sores. Ointments which contain zinc oxide for diaper rash are also noted for healing skin sores and rash-like skin areas.
Baby Powder
I sprinkle some of the powder into the front section of the diaper and a little on the skin exposed to urine. I find it difficult to use the ointment in the frontal areas. The plastic bottle with the powder will last over two months (cost about $3.00). I have had success with this procedure which appears more effective than using an anti-bacterial first aid spray that is sometimes recommended to cure frontal red areas bordering on infection.
Baby Wipes
These wet wipes are about 7" by 8" and are packaged in units of 80 or 160. They are a "must" to keep the buttock clean of urine and waste matter. My cost at the drug store is about $4.00 for the larger size. I find that soft paper towel sheets, like Kleenex Viva cut in half, serves conveniently in cleaning up solid waste.
Safety Features
I find that a small box of large safety pins is very useful. Sometimes, the adhesive straps on the briefs do not fasten, and a safety pin can be used for this task. However, be careful not to hurt your loved one in the process. When I started moving my wife, I found some bleeding scratches on her arm. They were caused by my rough belt buckle - which I soon changed. I obtained a belt that had two metal circles that I could thread the belt through which prevented these scratches. Also, look at pencils in your pocket or rough finger rings. I suggest you remove them when you move your loved one. I have heard of a case where a pencil damaged the eye of a patient, so take care to prevent these types of accidents
Under Pads
These pads are thin, absorbent sheets with a blue plastic under layer and a soft, upper absorbent layer. The sheets measure 22.5" by 35.5." They are placed under a patient to absorb any spillage out of the briefs during the night to protect the mattress. I use two with one slightly overlapping the other on the edge. There is 150 count in a box, and they will last about a month (cost about $60). The process of making the bed is discussed below.
Waterproof Bed Pad
These quilted pads protect the mattress as they are waterproof. I place one of these under the under pads for double protection. They are washable. Troubles resulting from the failure of the thin under pads are rare, but when they occur, you will have peace of mind knowing that the mattress is protected by the quilted pads. They have a soft cotton/poly top with a waterproof bottom face. Also, this quilted cloth pad serves the important function of moving the patient while the patient is in bed by grabbing the edge of the pad and pulling in the desired direction. Two of these units, 25" by 35" each, are desired for the bed (cost about $10 each, Dr. Leonard's Health Care 1-800-785-088). This type of pad may cost more, but their function proves their worth. As with all products I mentioned, I do not verify the product. They are ideas to follow-up.
Bathing Chair and Shower
Showering an invalid patient will require a movable plastic stool or bathing chair to sit on while they are in the tub under the shower. The one I use has two slots on either side of the seat for handles. These slots provide a hole that the wooden cleat from the bathing transfer board can be inserted into to connect the bathing chair with the wheelchair, thus providing a firm system for transferring the patient (discussed in detail in the Bathing section below). You may find other ways to tie the bathing transfer board to the bathing chair, so you may use a different chair than I use. The one that works for me is called Deluxe Bath Seat (21" W by 18" D with adjustable legs) with a back sold by Rubbermaid; it is found in the Dr. Leonard's Catalog, 1 800 785 0880 at a cost of about $60. A local health care store may carry one that might suffice.
In addition, you will find good use of a hand-held shower with its long hose that replaces the old showerhead. You may find it in the local hardware store at a cost of $20 to $40.
Toilet Chair
In some cases, the patient might not able to go the bathroom for the toilet needs. There is a white, plastic chair, with removable plastic bucket under the seat (cost about $ 80 in the local medical service store). This can be placed in the bedroom for convenience. Sometimes, a used one is available.
Clothing
This item is often overlooked. In planning for everyday clothes, what is needed is clothing that is simple, easy to put on and off and nice looking. Thus, the following suggestions in clothing. I dress my wife in stretch pants and shirt. If you dress the patient in bed, you must pull the pants over the briefs and tight pants do not work well. Using the right size pants so they can be easily slipped off to change the briefs is important. In my case, I buy pants that are at least one size larger than my wife usually wears, such as from normal to large. This will give you pulling room. They also have an elastic belt at the top some 1 ½" wide which is important. I grab the elastic belt by both hands when I move my wife from the wheelchair to the bed by swinging her onto the sliding board. The elastic belt makes the pants fit, so she is able to walk at ease. You will find a daily change advisable. It is a good idea to buy only one and try the new pants, before you add to the collection (K-MART had some reasonable priced pants and blouses for about $15 each). The shirt should be loose on the patient. In my case, I first slip the short arm sleeve of the shirt over arm that is paralyzed without trouble. Bright colors in the shirt help the patient's morale. Also, I dress my wife in white, ankle, half socks which I grab to swing her onto the bed when she is transferred from the chair to the bed.
BED AND BEDDING
The Bed
There is nothing unusual about preparing the bed, except you will need to add some measures of protection and accommodation. When the patient is in bed, you should provide protection from rolling out or getting out of bed. I place the wheelchair tied with a velcro strip to the bed where my wife sleeps. Also, I place another chair next to the bed which adds to the barrier. I find it convenient, as a right-handed person, to place my wife with her head to my left as I face the bed. This permits me to use my right hand to more easily remove waste and to straighten the briefs, but this is only a trifling task. Also, you should plan for a convenient location to keep the briefs, ointment, and wipes to be reached easily from the bed.
Preparing the Bed
After the bottom sheet is in place, I place a permanent quilted waterproof pad and two throw-away blue plastic under-pads in the area where my wife will rest. I overlap on the blue pads by about two inches to provide leakage protection with the quilted pad underneath to provide a final barrier for the mattress. The reason for overlapping the blue under-pads is that when I change a brief, I don’t accidentally pick up or move the blue under-pad as I’m sliding the wing of the brief under my wife.
Changing Briefs
It is possible during changing of a brief that urine or waste might spill over the brief onto the under-pad which requires removal from under the patient. This is an easy task. Simply, roll the patient on their side, roll the under pad into a scroll at the intersection of the edge of the back with the bed. Roll the patient over the under pad to their other side and remove the soiled pad. Then, place another pad in the scroll form at the intersection of the back with the bed and roll the patient over the scroll. At last, straighten the pad out. This technique also applies to the changing the brief on a person when they are in bed with the wings of the brief rolled into a scroll.
If my wife is too close to the edge of the bed, there is a easy way to adjust her position. I place my left knee against her hip with the right leg resting on the floor. I push gently toward the new location, a few inches inward with the left knee, using the right leg to help with the boost. I use this same method for to the upper part of the body as well.
TRANSFER
Moving your loved one between the bed or the recliner and a wheelchair is termed "transfer", and for the novice, this task maybe difficult at best and terrifying at other times. As I was leaving the rest home with my wife in a wheelchair, the chief therapist said in undignified terms that an 80 year old man could not match this task and to leave my wife in the rest home. I looked her in the eye and replied I must meet this challenge come hell or high water. I believed that with my personal care at home my wife would be happier. It turned out, I was right. So I left for the great adventure of home care. That therapist's caution made me edgy, which was good, as I took great pains to be careful in this endeavor, and you will benefit by my experience.
Velcro Strips to Attach the Wheelchair
Even though wheelchairs have levers to lock the rear wheels, the wheelchair still can slip, especially on carpet. Velcro can be a great friend in solving this and other home care problems. For instance, when moving my wife in and out of bed, we strap the wheelchair to the bed using a Velcro strip wrapped around the bed frame. I use a similar Velcro strip for attaching the wheelchair to the recliner.
Transfer Movement
I have used two general methods, the standing turn and the sliding board. These enable you to more safely transfer an invalid from one place to another. An example of safety practices is to grab the shirt of the patient with your hand when pushing a wheelchair. One unfortunate experience happened during a standing turn movement from the wheelchair and my patient slid to the floor. Of course, you may customize these methods to fit your condition. In both cases, I first secure the wheelchair to the bed or other chair using Velcro strips described above.
Standing Turn Movement
In the standing turn, you raise the patient from the chair to a standing position by pulling on both arms, turning her by moving both arms thorough 90 degrees, and setting her down on the locked wheelchair. I do not like this method because in the turn, you depend solely upon the patient to make the turn under your guidance. If she is unsure and can not balance herself she could slip or fall, as occurred in my case. Also, a hard pull may badly damage the sockets of the arms. However, a modification of this previous method is safe. Tell the patient what you expect her to do. With the patient's legs 90 degrees to the floor for assistance in standing, you can reach over her shoulder with both arms and grab her belt with both hands, raise her from the chair to a standing position, and turn her into the wheelchair. Prior to lifting the patient, I find it important to maintain a safe balance which is done by inserting one leg between my wife’s knees, and placing the other leg in the direction you wish to turn. Have your loved one look towards the way you are turning. You are in control all the time, and they will help the move by using their legs to lift their body.
Transfer Board Movement
Moving an invalid is truly a unique challenge which, I found, was only vaguely defined by home care specialists. This method is often referred to as the transfer board movement. If your patient cannot reliably use their legs, you will need a special board with a slick surface to move them between the wheelchair and the bed and to other chairs. These boards ranges in size from 8" by 24" ($35) to 8" by 30" with a hand slot ($54). The large size is the best. The slot is useful since you can easily hold the board when placing it under the patient. You can make one out of plywood with a taper on the end section and wax it or paint it, but you must make absolutely sure the surface is smooth and without the possibility of splinters. I have made one for transferring my wife in the bathtub, as I will relate.
To move my wife between a wheelchair and the bed, I first position the wheelchair and fasten it to the bed frame with Velcro strips and lock the wheels. I then remove the wheelchair arm closest to the bed. I then lay down a folded plastic sack on the bed where I am going to move her, which is discussed below. I then grab and lift the pants of my wife under her hip, and slide the tapered end of the board about halfway under her bottom, if possible, with the other end of the board resting on the bed. I check to make sure her feet are 90 degrees with the floor. I reach over her shoulder with both hands and grab the elastic web belt of her pants. Some therapists put a white wide web belt on a patient for grabbing, instead of using the elastic band. But I find the web belt hard to put on and hard to use as it slips a little. I have found grabbing the elastic band of the pants works fine. I bend her forward a little and lift her slightly, at the same time, move her towards the bed (or a chair) in a bouncing fashion. By sliding and bouncing her along the board, I incrementally move her onto the bed onto the folded plastic sack.
Pivoting – the black plastic bag trick
You will need to turn your loved one to lay her down in bed or put her into a car. There is a small turn table for this purpose (about $20), but I find it cumbersome to use. One of the best tricks I’ve found for this action is to fold a black plastic garbage sack in two and place it on the surface you will sit the person on before you lay them down in bed. Once the person is sitting on the folded plastic sack, with one hand grab the two half-socks of the feet, lift the feet gently in the air, and turn her toward the inside of the bed. With the other hand, steady her back while the turning action is taking place. The two plastic sheets easily slide between each other, making the rotation easier and keeping the underpads on the bed from moving. After this action is completed, you can roll the patient on their side and remove the folded black plastic sack.
Car Transfer
Perhaps, the greatest achievement and pleasure of the home care challenge was when I found a way to transfer my wife from the wheelchair to the front seat of the car. It meant freedom from the bondage of the house. You need to master this movement, so you can go to the doctors' office and travel on emergencies. There are two ways I have employed for car transfer.
The first is using yourself and the support of another person if the patient can walk a few steps and stand. I place the wheelchair as close to the opened, right front door, and tell my wife exactly what action she will be required to play and what I intend to do. I place her feet at 90 degrees to the ground, so she can help with the lifting movement. I take hold under the left arm and the other person takes hold under the right arm. At the signal, we stand her up and all three walk toward the front seat and stop in the space of the open door. It is important for her to be as close to the front of this wedge-like opening as possible so she can swing inward and sit on the front seat. The one holding the right arm places her right hand on the top of the door to give her assurance. The one holding her left arm slides his right leg under the upper part of her left leg to give support during the pivot. This pivot person grabs her mid section and swings (pivots) her on her legs under the roof and into the seat leaving her legs out side on the ground. At this same time, it is important that she releases her hand on the top of door to make the transfer complete. The one on the right side eases her head under the roof of the car, so she will not injure her head.
The last act is to place the patient's legs into the car and move the patient into the seat by pulling on the pants of the patient. This is easily done by reaching through the car on the driver's side. Be sure the seat belt is fastened and the patient's hands are inside the car, not in a place they can be injured when you close the door.
The second type car transfer uses one support person and a sliding board. You can easily make a suitable sliding board out of a piece of sub floor laminate which has a plastic-like, slick surface on one side. The size is 8" x 26" x 3/8". As an alternative, the board could be a little longer and made out of plywood with a slick surface. Before I proceed, I should tell you my dilemma. I am an engineer, and for over a year, I could not move my wife without another person for support. The large wheelchair we used would not fit into the space of the front door to get the sliding board in place for the transfer. I thought of many ways to overcome the obstacle, like modifying the hinges on the door, but that would call for welding new hinges and repainting.
One day, while talking to my neighbor, the physical therapist, he suggested I use his special small wheelchair which had moveable arms and a special sliding board which I have described. The special wheelchair has been listed under the preceding topic of "Wheelchair" for a source of supply; it is termed "Breezy by Quickie". It has moveable arms which is a very important feature and is only 16 in. wide; it also folds so it will fit in the trunk. Also, Dr. Leonard's Health Care (1 800 785 0880) sells a similar item, Sporty, Lightweight Wheelchair, with folding arms and is a portable wheelchair for $300. It may be marginal for use for some spaces in the front door space of some cars, so check it out by using a mark like a cutout cardboard sheet for the total chair width.
To execute the one person support movement, I place her in the special wheel chair into the space of the opened front door as close to the car seat as possible so I can work this space. I tie the wheel of the wheelchair to the car using a Velcro strip threaded through the hole that appears in the post of the door as part of the hinge assembly. I place her legs at 90 degrees with the ground, so they can help with the move. This, plus locking the wheelchair breaks, is extremely important to prevent the wheelchair from slipping out from under the sliding board that is mentioned in the next step. With the inside arm of the special wheelchair removed, I slide the sliding board under her in the wheelchair. Because of the conditions, the board may not move under the person as far as I may like, so it might be necessary me to slightly lift her onto the board before you do the sliding.
For the move, I reach over her right shoulder and grab the elastic belt on her pants with both hands. This points her head towards the inside of the car. If she can use their legs, I pull her towards me (lifting slightly) and swing her on the board in a sliding manner. The object is for the her to use her legs in the lifting and turning movement if possible. When she is on the board, I bounce and slide her into the car .If the board moves along the seat of the wheelchair and will likely go into the space, I stop and move her back, the way she came. I reposition the board and begin the same sliding operation. With her safely on the edge of the seat of the car, I lift her feet onto the floor inside the car. Then, as before, I pull on her pants to move her further into the seat and fasten the safety belt.
When you move the person out of the car, you will tie the wheel chair to the car post with Velcro strips in the same way as you did in the entering movement and lock the wheel brakes. Place both feet of the patient outside the car; the feet may not touch the ground, but will come into play during the movement. In moving her out of the car, I find it more practical to place my right foot inside the car, leaving my left foot on the ground. I am able to push with the right foot inside the car while the left foot serves to slightly lift her. I bend her forward and grab the elastic belt on her pants in the back with both hands, but his time I reach over the left shoulder so she will face the out side of the car. Of course, I lift and bounce her along the board into the wheelchair. I always watch for possible movement of the board which could result in her falling to the ground. I find it is easy to stop and check her movement along the board periodically to make sure everything is OK.
BATHING
 |
| Fig 3. Bathing chair with velcro strap. The climbing harness used for transfer is on the grab bar in the back. |
When she left, I realized this system would not work for us at all. Even two people (especially one who is an 80 year old 130 pound man!) cannot reliably use this method to move an unclothed invalid who also weighs about 130 pounds. About the same time that my wife left the nursing facility, a friend who also left the facility found that his bathtub would have to be replaced or modified with a special unit costing thousands of dollars. This also added much to my concern. I immediately decided to use my best engineering talents to get out of this mess, although I was not experienced in this field.
I needed two inventions to bathe my wife. The first was a special bathing transfer board that would provide a firm surface for transferring my wife from the wheelchair to the bathing chair. The second invention involved finding a way of holding onto her without the benefit of clothes or the elastic belt in her pants for the movement. For this I needed a bathing harness. I quickly found it is nearly impossible for one person to move a naked invalid around. I am aware of a situation where three men had a very difficult time removing an unclothed invalid from a tub when the person had fallen down. So I began the challenge by searching for ideas in darkness. To fail meant my wife could go back to the rest home. That was a real incentive to succeed.
Bathing Transfer Board
Here is how my bathing transfer board was made. This is not just a sliding board like we discussed above for transferring between the wheelchair and the car. It also serves as a structural beam to tie the wheelchair to the bathing chair and to interface with the tub. This provides a firm foundation for moving my wife from the wheelchair to the bathing chair to minimize the chance of falling. From 3/8" thick plywood sheet, I cut the outline of a sliding board which was 14" by 36". The large end (not trimmed) fit against the surface of the bathroom wall above the tub. The other end, used to slide under my wife, was reduced to 7" with the corners trimmed in quarter circles. This end was carefully sanded to give a smooth transition, in order that she would slide on to the board without difficulty. I cut a notch to fit the wheel of the wheel to permit the wheelchair to come close to the bath tub and to permit a small overhang to extend at least an inch onto the seat of the wheelchair when it is moved in place. You might consider using a large cardboard sheet from a large package box as a template to check the elevation and location of the assembly with the wheelchair, as the height of each part can vary for your particular situation.
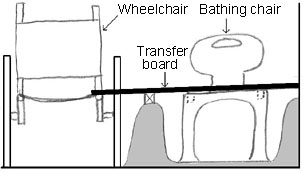 |
| Fig 4. Diagram of bathing transfer board set between the wheelchair and the bathing chair. |
To improve sliding, I covered the surface of the sliding board with a double layer of black plastic film and secured it with fiberglass tape. The tape holds the sack in place under wet conditions. I am sure a good paint waterproof paint would also suffice.
Bathing Harness
A little background will give you an appreciation of the difficulties in finding a way to move a naked invalid into the bath. Obviously, using a towel under the armpits to lift a person is rather crude and unsafe for the layman. I was surprised that the local medical equipment store did not have any kind of a harness for lifting a person into the bathtub. After some thought, I decided that I could make a harness with two leg loops which could be fastened to a belt to give enough places to hold for sliding a person across the transfer board. Off I went to the local fabric store with a sketch of a harness to find the straps and rivets for making this assembly. I wanted to recheck my plan with my friend, the specialist on geriatrics, so I returned home. She listened and said, "Why do all that work, just go to an outdoor sports store and buy a rock climbing harness!" And I did with the feeling that as an engineer, I had been truly outsmarted. Why the medical profession does not make use of this simple low cost device to move unclothed patients remains a mystery. To me, it is the best invention since the wheel for moving an unclothed person safely. The rock climbing harness is very well made and costs about $30 (REI, Recreational Equipment Inc. Salt Lake City, Utah, 800-426-4840 or 801-486-2100).
Bathing Process
 |
| Fig 5. Flexible shower head |
The reverse operation is used to get her back to the wheelchair. During the bath, we wash her with soap and sprayed water from a hose attached to the shower head (Figure 5). If you place a wet wash cloth on the sliding board between the edge of the tub and the patient, water running in that direction will drain inside the tub.
I have successfully used this method without any kind of accidents for about two years. It is a relatively easy way to bathe my wife, but I emphasize that care must be taken in bathing to prevent serious injuries. It is important to use safety measures. The bathroom is very hazardous place for falls, so be on guard.
RECORDS
This area is difficult to manage for non-scientific people; in fact, I have experience this trouble myself, and I am an engineer. Much of the following information was gained by trial and error. Thus, you may profit by my mistakes. Of all, the most important is to keep a daily record on the patient. Healing is a slow process, and you will have a hard time telling if you are gaining or losing by daily monitoring. It seems best to review the progress over a matter of weeks. Here are some of the records I found very useful in the care of my wife.
Blood Pressure
A reading should be taken each day at about three times a day at the about the same time each day and under the same conditions (location) to get some kind of a standard. I took these readings until I felt the pressure was under control. Then, I would occasionally spot check the condition. Example: I found the readings would reach as high as 170 systolic (very rare). Mostly they would be below 140 and were satisfactory. I wanted to know if they would be in the 170 range because high blood pressure can break blood vessels and lead to a stroke or heart problems. If the reading is in the 80 systolic range, there is also serious trouble as not enough blood goes to the brain and the patient can faint. In my wife’s case, satisfactory upper limits are a diastolic less than 85 and the pulse rate less than 80. Be aware of very high and very low readings. Talk to a doctor about this condition as soon as possible. A high rapid irregular heartbeat (pulse rate) is also serious as it does not pump much blood.
Temperature
A reading from 96 to 99 is a normal range on the thermometer; above 100 indicates trouble like fevers such as the flue. In the range of 104, the condition is serious, so call a doctor. Do not wait in this serious condition; get the temperature down with cold packs at the doctors instructions. A rubber (cold or hot) water bag with its removable lid can be obtained from the drug store which can be filled with water and cooled for cold packs.
Daily Records
This record should record the condition of the exercise such as "walked with two people around the room two sessions 10 times each; my wife continues to lean to the left." Daily records should show if the patient sleeps or does not eat, or some other change from the normal status. This information becomes important showing a trend in the weekly review. When my wife would sleep a lot and only walk a few steps, say 5, I knew that a mini-stroke had struck. I was in trouble and needed help from the doctor to change the care. Keep notes on the medicine such as starting, ending, increasing the dosage giving obvious results (like dizziness) if possible.
Monitors
The monitors that should be on hand to determine the patient's condition. My units are the thermometer, like BD Standard Digital Thermometer and the blood pressure monitor, like Omron Digital Blood Pressure Monitor HEM 412C. These are not expensive and can be obtained from the local drug store.
MEDICINE
Providing a patient with the doctor's prescribed medicine is essential to improve the patient's health, and in some cases where there is difficulty in giving the drug, it can be seriously overlooked. Thus, a system must be established in advance of giving the medicine on the first day a person arrives home. I find the medical book, The Mosby Medical Encyclopedia, (cost about $20 at the local book shop) with its easy-to-understand terms very helpful in talking with the doctor about difficult health problems that may appear in your caregiver assignment. I have chosen to discuss vitamins and the like under the subject of health, as it is from foods and vitamins that our bodies get sustaining chemicals for their function.
Dispensing Medicine
Here are some lessons that may provide a guide for this activity. A note with our prescription drugs was challenging: about 30 to 50% of those who use medicines do not use them as directed. You should find out specifically what each drug does to the patient and try to register how well the drug is doing. Example: if the patient is taking aspirin to thin the blood after a stroke (or heart attack) and the patient has a mini-stroke, it is obvious it is not functioning, so talk to the doctor. Somewhere, keep a list of the drugs and the specified time they are to be given, if required. A pill dispenser box may be obtained from the drug store to help keep track of the drugs you are to give the each day. The drug store has a pill divider and a pill grinder to powder the pills for those who need these specialties. In my case, my wife does not like a pill so I grind each one up and dispense it in a spoon after mixing it with a little water and adding a little grape jam. The sugar makes the medicine go down.
Characteristics of drugs
It is very helpful to know the characteristics of the medicine a patient is taking, so you may understand its purpose and such attached problems as side effects (examples: sleepiness, vomiting, bleeding, headaches, or rashes). To know about the drug that the doctor has prescribed, look for it in the book, THE PILL BOOK ($27,), Bantam Books, 1540 Broadway, New York, N. Y. 10036 or in your local library. In some cases, you should not mix types of medicine. Also, the book talks about the generic name to lower costs, type of drug, prescribe for general information, cautions and possible side effects, drug and food interactions, usual dose, over dosage, special information, special populations, and seniors. Thus, if the patient has some dizziness after taking medicine, you can talk to the doctor in real knowledgeable terms to manage the problem. In this respect, a doctor once told me that a significant number of calls for medical attention were due to the side effects of mixing medicines. An important source of medical assistance is the local pharmacist. I found my pharmacist, Clifford Hold, was very helpful with such problems as poor bowel movement, urinary track infection, irregular blood pressure, and healing bad skin cuts as a result of wheelchair movements. The pharmacist will handle the serious problems with your doctor's instructions.
If the drug is not working by its performance, do not be afraid to talk with the doctor. For example, if after a stroke, the patient has a mini-stroke, it is time to change something...obtain the best advice or you can loose the patient. And if the doctor is difficult to reach, from my view, still attempt to reach him and talk it over as he may have too much on his mind that day; change conditions only after thinking your situation is in the best interest of the patient, not the ego. I find most seniors are interested in taking an aspirin as a blood thinner to prevent strokes and heart attacks. The government paper, Collaborative Meta-analysis of Randomised Trial of Antiplatelet Therapy for Prevention of Death, Myocardial Infraction, and Stroke in High Risk Patients tells much on its website: www.pubmedcentral.gov/articlerender.fcgi?tool=pmcentrez&artid=64503 showing the results of using aspirin for this purpose. Aspirin is protective in most types of patients at increased risk of occlusive vascular events. It says that daily aspirin doses of 75-325 mg are effective. Talk to your doctor to determine if there could be problems in your case.
Bed Sores
The preventive measures for sores is to change the briefs when it is required, to apply ointment and powder to the areas exposed to urine, and move the patient about to change the pressure points at long rest periods. Following this procedure, I have not had problems. Rest homes move patients into the wheel chairs to change the patients position as one of the preventive measures. If sores appear, one of the better treatments is to apply "Bag Balm" which is used to treat this condition on the bags of milk cows. It has worked well for me for healing sores. This product is made by Dairy Association Co., Lyndonville, VT, 05851. Coast-To-Coast and other hardware stores along with some department stores carry this product (cost about $ 4.00).
DISASTER STRIKES
Unfortunately, you will likely experience a fall on the floor by the patient. Most of us with seriously handicapped patients have had this misfortune, and there seems to be no straightforward method of getting the patient back into a chair with one guardian. Even therapists witness this fact of life. The hospitals have a special lift to move invalids out of bed which can also be used to handle people who have fallen on the floor. Home caregivers do not normally have this luxury. The first action to take when you see a patient slipping is to try and break the fall, so no bones are broken. Most of my experience with this problem has been on a carpeted floor, and my luck held with only one related trip to the hospital in two years.
One Person Available
Now, I will tell you some of my experiences, so you can be on guard. A couple of times, my wife put her legs over the bed to get up by herself and fell on the floor. Upon discovery, my heart sank below the foundation of our house. Then, I took measure. At this point, I did not move her because a broken bone is serious and can cause complications if the person is moved. But nothing was hurt, only her pride. Now, it was a challenge for me to get her back into bed, and she weighed as much as myself. I performed this task by raising the body parts onto the bed, one by one. After I straightened her with the back leaning on the bed, I turned her on her side to the bed and brought the legs along side the bed. I raised the left arm and the head to the height of the bed, holding them on the bed with my left leg, left hand, and a push with my body trunk. This turned the her face and body somewhat inward toward the bed. Then, I raised the other arm (right arm) to rest on bed, still holding her body trunk up with my left leg. Next, I raised the right leg by crossing it over the left leg and placing it on the bed, at the same time pushing the right arm inward. It is kind of a rolling motion to get her on the bed nearly face down. At last, you keep the rolling action going by lifting and forcing the left leg on the bed which is the heaviest part as the remaining trunk is rolled onto the bed. To get the patient more to the center, pull inward on the cloth waterproof underpad. If this appears complex, it is, but you must do something. Thus, you wind up putting each body part with the weight you can lift on the bed at different times. This taught me a very good lesson in safety, and now I tie the wheel chair to the bed when I leave, providing a barrier.
My neighbor told me that she lifted her husband into bed after he had fallen on the floor by tying the ends of a towel together and placing it under his armpits, and then pulling him on his back into the bed. It seems to me that you would need some help from the legs of the patient in this case. Also, the backbone could be damage, and I do not recommend it. Use care and thought on these kind of moves.
Two Persons Available
Sometimes, whatever you do, you can not stop a fall, but try to make it a soft landing. Several times over the past two years my wife fell to the floor while walking during her exercise with a person on each side. If we see by her steps that she is tripping or losing her balance, one person will immediately slide the upper part their leg under her to provide a temporary stool. This allows time for the other person to get the wheelchair. We then grab her under the arms and lift her into the chair .My friend in geriatrics figured this one out, and it has worked well.
If this does not work out, we let her settle to the floor, put her in a sitting position, and get the wheelchair. With one person on each side, each grabs the belt on her pants a little in the rear, and puts their other arm under her armpit. At a signal, we lift her into a chair. Her legs can take some of the weight, while the remaining weight can be easily handled by the two of us. If you are alone, and you can get a kind neighbor who has the strength to lend a hand, then use this last method to get your loved one off the floor, if there are no broken bones. A call to 911 will certainly bring help. However, my use of that important service in Evanston, Wyo. cost nearly $300 and in Pinedale, Wyo. about $550. But that is sometimes the cost of doing business.
Lifts
I should discuss a mechanism used to raise an invalid off the floor, out of bed, or other necessary functions. In the nursing care industry it is called a "lift." Because it is a bulky, expensive machine you will find most of them in the hospitals. The cost ranges from $900 to $1250 new and about $400 to $500 used (Praxair Health Care Services, 801 261 5100). I was told to wait by a home care specialist until I was sure I could not handle my wife before I made this investment. A brief description of the lift that I have seen can give a better view of the operational problems. The front is an extended circle with rollers and at the base of this unit in the back is a set of rollers. Extending from the back is a post with an arm which by cables and a sling are used for lifting a patient. One of the problems is that its size makes it difficult to manage in close bedroom spaces. If you think you need one of these, take good measurements. I was able to move my wife by the sliding board and the assistance of my geriatrics friend, precluding the use of a lift.
HEALTH AND WELFARE
This section is not intended to encompass all health items but to familiarize you with some essential ones as I see them. I will discuss them separately.
Alzheimer's Disease
Prior to March, 2002, Medicare coverage was denied to over four million people for mental health treatment, hospice for the dying, and home health services because they had this brain disorder not of their making. Shame on those officials for denying treatment to those people. After all, they paid their social security taxes for this entitlement.
Since many of the old people fill our wheelchairs, I should discuss an aid that could reduce the fear of Alzheimer’s disease with these people. The New England Journal of Medicine published an article some time ago which gave the results of testing some 1000 older people by medical researchers from Boston and Tufts Universities. They found those with high amounts (over 14 micromoles per liter) of homocysteine, an amino acid, in their blood were more likely to have Alzheimer’s than those with low levels of this acid. The best way to counter this serious problem is to increase the intake of foods and vitamins with folic acid. These people need a daily minimum of 400 units of folic acid in their diet. Green vegetables, beans, orange juice, enriched bread and vitamins (B vitamin series) are some sources for folic acid. To show the importance of folic acid in the diet, I will cite the success of the Food and Drug Administration’s program of having mothers take folic acid during the time they are carrying their babies. Since 1998 nerve tube defects (like spina bifida or back curvature with a gap in the bone around the spinal cord) in births has dropped by some 20 percent. Thus, folic acid is highly recommended for mothers with unborn children.
For your information, I would like to relate a personal experience with the lack of proper diet by older people. My mother (72 years old) was maintaining her home alone and could not get up from a fall on the floor; fortunately, my cousin visited her often and discovered her accident just in time. After medical analysis by Doctor Donald Smith in Salt Lake City, she was treated for pernicious anemia by taking vitamin B-12. This case resulted in loss of mind similar to Alzheimer’s. She was stabilized and placed in my care, but never regained her mind. She died 5 years after this event. In summary, I think it very important for older people to track their use of vitamins and at least take the correct amount of critical ones like folic acid and vitamin B-12. Check with your doctor for approval and help.
I would like to discuss the application of vitamins and trace minerals in aiding victims of stroke and seizures (convulsions). Of course, this type of nutrition can apply in all cases of health improvement. My wife has had both of these unfortunate occurrences. The gerontology specialist said that this connection of the strokes with the seizures is not uncommon in older people. When there is a stroke, the nerve "wiring" and electrical signals in the brain are disrupted resulting in paralyzing parts of the body, like my wife’s left leg. But greater powers have taken care of this in time, permitting the body to rebuild an associate system in the brain that enables the person to walk again. Thus, the therapist in Jackson was wrong in her judgement that my wife would always be an invalid, since she is now walking by her determined mental prowess and her nutrition. Mark Bricklin’s book, The Practical Encyclopedia of Natural Healing, relates that in epileptic seizures the GABA (amino acid) gets low in the brain and the body loses control over the brain nerve cells (neurons). These cells become electrically hypersensitive and discharge at a rapid rate promoting a seizure. I can tell when a seizure is likely to happen to my wife as her left arm, paralyzed by the stroke, begins twitching and jerking. I then give her a glass of tomato juice with its high natural potassium. In our case, this normalizes the movements. When my wife has a seizure, I hold her close to me and encourage her.
Electricity in the cells is a very complicated matter. We know that an element or compound when dissolved in water breaks up into ions capable of conducting current in the cells. This is told in The Mosby Medical Encyclopedia, which I recommend for excellent home care reading. Since the body is roughly 60% water, it is easy to see that when food, with its various molecules is consumed, electrolyte compounds are formed that affect parts and functions of the body.
An example is potassium. Its compounds in critical proper amounts are needed in the nerves to contract muscles and relax the heart. Various body functions also occur with other trace elements and their compounds, like magnesium, manganese, including the B6, and choline vitamins which have a chemistry related to seizures. Well-known elements, within their correct limits, are calcium for heart muscle action and sodium for fluid balance. Both play a role in good health. You can see that chemicals influence the signaling in the nervous system. An example of this function is the famous "calcium blocker" pills, which control high blood pressure in older people like my wife.
Potassium is needed by plants and animals to live. Heart doctors insist on the control of sodium (salt) in the diet of heart patients. This short discourse on body chemistry is included so you will know the importance of taking vitamins along with the drugs and food that contain the products to overcome deficiencies that create health problems for older people. My wife in her stroke condition is given a vitamin B complex including folic acid to promote recovery of her nervous system and to aid in converting food into much needed energy. Her vitamin C is an antioxidant to contain free radicals and aid in cell repairs. Her daily intake of a banana provides the potassium for her deficiency. In my wife’s case, food is mashed for easy eating. With these aids, I have seen improvement in her daily performance. Any of these aids that benefit the nervous system are important in containing Alzheimer’s. After reviewing this information and the patient’s blood profile, I recommend you talk to your doctor to plan the best health improvement program for your patient.
Welfare of the Patient
Being bedridden can create hopelessness for a person, and it is necessary to brighten up this condition for survival. I suggest a few things that can improve this bleak experience. Dress your loved one in bright clothes every day. Music (like classical which has an easy pattern) from the radio, selective TV programs, VCR movies, reading to the person, encouraging someone from the patient's church to visit, encouraging friends and relatives to come to the house, and transferring the person to the table at each meal to make life a home style setting are some of the helpful activities to enhance your loved one’s mind. But to me, laughter is also very important in all the cures.
I sense that the strongest influence on a return to good health is faith. It is the immune system that plays the largest role in this healing process, and faith stimulates the body's chemistry toward this goal when it is employed. When you feel badly, you may shed tears which illustrates the point of energizing body chemistry. This thesis is supported by Rachel Zoll, Associate Press writer, as she wrote in her column (date not available), "Repeating a prayer can lower the heart rate, breathing rate, and brain wave activity according to medical experts." Also she wrote that Dr. Herbert Benson, professor at Harvard Medical School, said that the mind could work like a drug, especially among people who had a strong faith in God or higher power. So do not overlook this source of help when you are in trouble. It has worked well for me in my troubled days, and it will for you.
Stress
Now, I should say a few words about stress which is not clearly defined because it deals with the mental state. This affliction applies to both the patient and the caregiver. I have often heard the words: stop worrying after something is amiss. How do you do that?
Here is the medical analysis from an article published in the New England Journal of Medicine based on testing 39 heart patients. More than half were affected by mental stress. This decreased the blood flow to the heart muscles and increased the blood pressure. But the heart rate remained well within a normal range. This has a long medical name, but it is linked to great risk of heart attack or sudden death from heart disease. Strangely, my family history has a linkage to sudden death and I have wondered why.
On this subject, I would like to report my health findings on pessimism and depression. Dr. Daniel Mark (heart specialist at Duke University) said from his studies of 1,719 cases that when people give up and feel they are not going to make it, it's usually a self-fulfilling prophesy. Pessimism appears even more damaging than depression which is shown to be bad for heart patients. Dr . Nancy Fransure-Smith (Montreal Heart Institute) gave psychological tests to 222 heart patients. Guess what she found. Those with the high score on sadness and depression were 8 times more likely to die within the following 18 months of the test than the happy warriors.
Laughter
I will turn to the obvious in a successful treatment program, laughter. In far off Sweden, Dr. Lars Ljungdahl studied 6 women suffering from muscular-skeletal disorders and depression. They were in his clinical program that did homework on studying the priority of humor in the daily life, rating funny things from a grin to a hearty laugh for a scale of five. Pain did not quite vanish, but the quality of life improved.
Here is another experience of one of the big guns on the subject of laughter. Norman Cousins in his book, Anatomy of an Illness, told his fight with death and his healing episode. The specialist in his case said Cousins' chances of survival were 1 to 500!. Cousins' reputation reaches from being editor of Saturday Review to senior lecturer at the School of Medicine, University of California. His disease was Collagen illness; the fibrous substance that binds the cells together was deteriorating, giving pain to all parts of his body. He studied his problem and decided that positive emotions produce positive chemical changes in the body. Emotions such as laughter, hope, faith, love, confidence and the will to live were studied from Hans Selye's book, The Stress of Life. In the duration of his sickness, he was served and supported by Dr. Hitzig, a competent M.D.
Part of Cousins's theory for recovery was tested by viewing funny movies. And it worked, as 10 minutes of deep belly laughter gave him two hours of painless sleep. Later, he also received doses of vitamin C. This is not bad. In my studies, according to Linus Pauling, the famous chemist, vitamin C is instrumental in holding the cells together. But Cousins was a scholar, and he wanted data on proving the positive effects of laughter, so he along with Dr. Hitzig used the erythrocyte sedimentation rate (ESR), which gave the rate and distance which red blood cells settled out in a tube of unclotted blood. Elevated test rates indicate inflammation and Cousins had plenty with his disease. They took these tests just before and several hours after the laughter periods. Behold, the test showed a drop of at least 5 points each time. And it held and was cumulative. This was the proof he looked for, which said that laughter is good medicine. They also took a sedimentation test 4 hours after the vitamin C was given. That also worked, dropping the test score some 9 points. He began to sleep, and after several months of this treatment, he was able to return to work (Anatomy of an Illness, p.40 and 42). Eventually, he became a medical specialist lecturing at the University of California. I have included this technical data to show humor plays a very important part in your home care treatment.
First Aid
The elderly have very thin skin layers and sometime they fall against the wall or brush against the padded wheelchair arm and peel the very top layer of skin. In my case, my wife received an accidental two inch skin peel of the top layer of her arm by the wheelchair. I called my friend, the therapist, who helped me with the problem as his wife had had a similar accident. I first taped the peeled skin back in place using a special tape called Nexcare Steri-strip (local drug store) which are 1/4 by 4 inches and perform like long term stitches; they remain in place during the healing process. Then, I used Neosporin to disinfect the area and covered the peeled area with a 3 inch gauze pad which was held in place by a special elastic rolled bandage. This bandage was non-sticking to the skin and fastened by over lapping the self-locking bandage.
On the second day, puss occurred in the broken skin which was disinfected by using cotton balls dipped into hydrogen peroxide (drug store); there was a little foam in the infected area. Beneath red areas is usually infection which can we controlled by the hydrogen peroxide treatment. It took about a week to heal the skin damage. However, if infection appears to be present, I am told it could lead to serious blood poisoning, so we would contact a doctor. Naturally, if the wound is bleeding badly, we would immediately go to an emergency doctor.
Dental Health
I have found it very difficult to keep the teeth of my wife free from decay. The elderly tend to keep food in their mouth after they eat as a way of life. This is bad for dental health, and the food residue should be removed after eating, if possible. I was not able to visit the dentist with my wife for nearly two years, and after a dental examination, she had 5 cavities. I then revised my program of brushing her teeth.
I first put a plastic bib on her which I shape into a bowl in the front with clothes pins to capture water and residue from the cleaning activity. The bib rests on the tray of the wheelchair. I then use a clean soft brush to lightly go over the inside of her mouth to remove food particles. I brush my patient's teeth with regular toothpaste using an electric toothbrush with soft bristles (cost about $8.00) which is a very effective way to clean teeth. I then use a water pick to clean out the leftover toothpaste and residue. Water from this treatment runs into the plastic bib.
Then, following the instructions of our dentist, I place a little fluoride toothpaste on the tip of a regular brush and go over the teeth to just cover them with the special fluoride paste. Roughly, this takes a large fluoride drop in each of four separate brushings, and I leave this small amount of fluoride on her teeth; but check this procedure with your dentist. According to our dentist, I need to do this to harden the surface of the teeth which will reduce the large number of cavities my wife suffers.
One main reason we need to perform a wheelchair transfer is to get my wife to the dentist. It can be difficult, but not impossible to maneuver the wheelchair in the dentist’s office. It is just another of the everyday challenges.
Food
If you are looking for information on food and diets, I recommend the book by Sheldon Margen, M.D., The Wellness Encyclopedia of Food and Nutrition, written in conjunction with the editors of the University of California at Berkeley. I would like to review some of the more important areas of nutrition which can effect you in care giving.
Removal of waste from a bedridden patient can be a serious health problem. Following a trip to the doctor with my wife regarding this matter, I studied the different ways to prevent a recurrence. This was cost savings in doctor's expenses. In my case, I found that a half of glass of prune juice with pulp at bed time and one in the morning see to activate my wife’s system to remove the waste when it is required. If this is not successful, I try 3 to 4 tablespoon of Phillips Milk of Magnesia on the third day. Fleet has a Glycem Suppository laxative that will also work well in this later case. The nice thing about prune juice is that it provides such good nutrition as 540 mg of potassium per glass, and it is possible that my wife’s deficiency of potassium could be part of the cause for her seizures.
After I gave this problem proper attention, the seizures have been controlled. Potassium within proper limits seems to be a "must" for the nervous system to function properly. It is useful to see what the blood profile tests show. For example, if the potassium count is low, then we eat foods that will tend to fill in that requirement. Your doctor should advise you on any deviations from the normal. A good way to help elimination of waste is by eating a fiber (like All-Bran cereal) in the morning. Much of the fiber is insoluble and absorbs water like a sponge producing a larger, softer stool for easier discharge. Note that fruits and vegetables also contain this good fiber.
Caution is advised in serving foods to heart disease and stroke patients; they need to maintain a proper blood supply through the heart and veins, and the type of foods they eat can affect their health. My studies indicate that we can profit by a significant reduction in the consumption of saturated fat. And Andrew Weil, M.D., tells in his book, Spontaneous Healing, that the biggest dietary mistake you can make is eating too much of the wrong kinds of fat.
However, fat and carbohydrates are stored for energy production, and we need them. The undesirable kind is saturated fats found in animal meats, milk products, coconut oil, palm kernels, and partially hydrogenated oils like those found in vegetable shortening. Look on the label to identify the amount of saturated fats. Weil also dislikes polyunsaturated fats because when they are heated or treated with bleach they turn into trans-fatty acids which can become toxic compounds. Good fats are from such sources as olive, canola, peanut, and avocado products. He recommends restricting your intake of fats to moderate levels of 20 to 30 percent of the total calories.
Briefly, fat molecules can react with oxygen and turn into free radicals (unstable) which react with other fat molecules, creating more free radicals. This wild molecule can damage the DNA and other normal functions of body chemistry. To prevent this mischief, the body has some antioxidant enzymes (SOD, GSH, and catalase) for this purpose, but with large numbers of free radicals, they can not handle the problem. Thus, to neutralize the excess free radicals, vitamins A, C, and E are often employed. It is not unusual for people in need of this dietary supplement to take 25,000 units of vitamin A (Beta Carotene) and 1000 units of vitamin C, but it is best to check with your doctor or druggist to effectively fit your diet. An informative discussion of free radicals and health appears in Dr. Kenneth Cooper’s interesting book, Antioxidant Revolution.
In another area, diabetes is a health risk. To decrease veins, heart, and stroke problems we limit our sugar (sucrose) from soft drinks and the like to 5 percent of carbohydrate calories. Soft drinks drive the blood sugar up too quickly hurting the digestive system. Fruits, beans, and vegetables are the ones to eat for unrefined sugars.
When my wife was sickly and not eating well, I would give her an energy drink, like Ensure, Boost, or Slim-Fast. I have found that even after I shake the can, there is nutrient resting on the bottom. So shake it well to gain the full health value of the nutrients. This adds some 230 calories (energy in a can) along with much needed minerals and vitamins to her diet. Some doctors recommend a "one-a-day" general vitamin and mineral tablet for old people. I supplement the drink with fruit and vegetable juices (natural vitamins) along with water. This activity carried the day, and she soon regained good health.
Providing water or other liquids to my wife when she was laying in bed was a challenge. The liquid was easily spilled, even though she was trying to drink. The solution was to use the small plastic cups that have snap-on plastic tops with a small spout. These are used to help babies or very small children learn how to drink and are available in almost any grocery store that sells baby foods. This allowed the amount of liquid to be controlled, allowing my wife to drink naturally, but also minimizing the possibility of a spill or other mess.
Exercise
Exercise is one of the most influential programs for the health of a loved one. To better illustrate the value of exercise, it is best to tell a brief history of my wife’s experience. She was about 82 at the time. It started in the Jackson WY hospital. My wife walked in the hospital preceding her kidney stone operation, but unfortunately, during the operation, she had a major stroke and could not walk after the operation. If the doctors had given her a special drug called tPa within three hours, the blockage would have dissolved, but his did not happen. Remember for a serious stroke you have only three hours.
In the following month, the hospital therapists gave her exercise treatments for her left arm, leg, and speech, concluding that they could not do anything in her case and therefore Medicare payments for further assistance would stop. This decision struck terror in my heart; being bedridden for the rest of her life was unthinkable. For many times after, I remembered those famous words of Gene Kranz, Director in the NASA space program, "Failure is not an option."
I transferred her to the hands of the more experienced therapists in Salt Lake City, and in their care she walked a couple of steps within the next week or so. It was the most wonderful feeling to know all was not lost, and that there is hope for everyone in this tunnel of agony. After two more months in the recovery home, Greg Cook, R.R.T. showed his expertise as a therapist by walking my wife some 400 feet in one day. This event served to facilitate the beginning of home care.
Upon arriving home with my wife in a wheelchair and with her personal belongings suited to the stroke condition, I obtained the help of an aid and we began our recovery phase. Within 5 days, with me on one side and the aid on the other, we walked her three times around the front room. It was the beginning of a long trial in patience. It was a bumpy road with sleepy days and sickness as the medicine was marginal, but within nine months my wife was walking around the front room some 120 times, resting at each 20th round. In fact, the aid had her walking some four times around the room alone with no support.
Just as this miracle of independence in walking appeared, she had another stroke and the nightmare in home care reappeared. This was about a year after we began the exercise program, and truly heart breaking as she lost had her ability to walk. I stopped and thought: I can not run the old Model T Ford at 60 mph and expect the head gasket to hold the pressure. Thus, we cut the maximum rounds to 50, and changed the medicine. The aspirin (blood thinner) was increased to 320 units for containing the stroke condition, and the sulfa drug was increased to a daily dose which eliminated the UTI (infection). In a similar case, you will naturally want to talk to the doctor before changing the medicine, as she may have knowledge of complications from the new procedure. I learned an important lesson for any exercise program to follow. You should use common sense.
Again with determination and faith, we restarted the exercise by encouraging my wife to stand in front of the chair 6 times on a Monday. It was slow but from that point she was able to take 25 steps by the end of the week. By the end of the month, we had my wife walking 13 times around the room, resting at each round. It was 5 1/2 months into this phase before we reached a target of 5 sessions of 10 rounds each in exercise. A year into the new walking program, my assistant can lead my wife around half of the time, holding only wife’s extended hands. On some recent occasions, we were able to just hold her belt in the back during 5 rounds of the walking session. So she is regaining her balance, and I am on cloud nine again. The case of a serious stroke is not hopeless as witnessed by this performance. This exercise has greatly helped my wife, as she is much stronger, does not sleep all day, eats well, and communicates. Why do I include the details of our exercise program? I have given you some of the troubles you may expect, showing the patience necessary to improve the quality of life for your loved one.
Now I will discuss the merits of exercise to provide an idea of the expected health improvements for your patient. Dr. Andrew Weil’s book, Spontaneous Healing p. 187, gives an excellent summary of the benefits from this source. These are listed: 1) improves circulation, 2) makes the heart muscles more efficient, 3) promotes elasticity to the arteries in the pumping operation, 4) enhances exchanges of oxygen and carbon dioxide with the air by the lungs, removing metabolic waste, 5) promotes the flow of perspiration ( waste removal), 6) moves the intestines (aiding release of stool), 7) improves mood changes and promotes relief of stress, and 8) helps the immune system. He also wrote that exercise generates electrical activity in the brain that has a harmonizing influence on the entire nervous system.
This excitement is just what I needed to stimulate my wife in her stroke situation. She is walking now whereas the first specialists said her case was that of an invalid. And now you have the successful reasons for my walking my wife. I have taken her blood pressure before and after each walking session and some typical numbers are: 143 systolic, 70 diastolic, and 85 /min. pulse rate (ending), 131 systolic, 75 diastolic, and 75 /min. (beginning). This shows that the entire blood supply system is energized. In addition to exercise, Dr. Weil added this advice: you need a good nights rest! This makes good sense because the red blood cells are made in the marrow of the bones mostly when you are sleeping. These cells carry the oxygen to all parts of the body, providing their energy for life. In conclusion, I firmly believe you should walk or exercise your loved one, if possible, to give her health, quality of life, and longevity. Also, this program will greatly relieve the burdens and anxieties of the caregiver.
I should mention my troublesome experience of exercising in the recovery home following my wife’s operation. The Medicare rule that the therapists must follow is that the patient must show weekly progress in treatment, or Medicare stops payment. This can be the beginning of the end for those in serious trouble and compassion does not play a part. With the stroke that followed the operation, my wife was in deep trouble as she was physically unable to walk according to the Medicare plan. She was always sleepy and weak. I would employ ice water in wiping a wet towel on her face to get action in walking, and it worked. When I finally had time to look in the drug (pill) book as to the side effects of her morning medicine, given before the walking started, I was startled. Her medicine was Celexa for depression with side effects of drowsiness, tiredness, and weakness. The other troublesome drug was Norvasc for high blood pressure with side effects of sleepiness, weakness, and dizziness. The doctors were not talking to the therapists. With persistency and ice water, I enjoyed the wonderful feeling of success on the day she began walking which continued the Medicare assistance. Thus, I caution you under similar conditions of therapy, identify the drugs and act accordingly.
Caregiver
Something should be written on the health maintenance of the caregiver since without this person in action 24 hours a day the home care program is jeopardized. This program is stressful, what with lifting and moving a loved one, lack of solutions for urgent medical problems of the patient if you cannot reach a doctor, lack of money to pay bills including hospitals and drugs, lack of contact with people, lack of sleep and eating properly. The list could go on especially for the aged.
It is important to occasionally change the daily routine. Consider hiring someone part-time to relieve you of your duties, so you may enjoy a coffee break with an old friend. If the chores are overwhelming, there are agencies that offer hourly, part-time services which will help you and still reduce your costs. What are other ways to enhance the life of the caregiver? I will give you a personal overview of choosing ways to ease the caretaker’s burden. Organize your day with a list of items to do and food to pick up from the store; keep emergency and other important numbers on hand. If food preparation is a problem, use Meals-on-Wheels. They will bring a meal to the door, providing there is any money left in the U.S. Treasury.
The Senior Citizen Centers provide a great lunch, interesting entertainment, and outlet for hobbies. They are a place to make friends with those with similar problems and solutions. Have the children call every other day or so to show that someone else cares too. There are volunteer services for those in dire need; they are under direction of the county aging services outreach program. Also, try local church programs, a relaxing video picture, books from the library, and the one I found best was research on the Internet.
At times, you may require the one day service of a care facility to "baby sit" your patient in the when you are called away on an urgent mission. I take my hat off to the nurses aids in care facilities who, in my experience, I have found to be competent, efficient, overworked, and kind to their patients. They normally attend to about seven patients which takes much patience to handle the many chores.
The key for success in the operation of home care is to remember that "failure is not an option." I can attest to this proven guidance. When events are very difficult, there are those saintly people nearby who will always help in your crisis.
